Home Health Essentials: The Ultimate Checklist for Managing Chronic Illness

Home Health Essentials: The Ultimate Checklist for Managing Chronic Illness
Transitioning from a hospital setting to home care, or managing a long-term chronic condition, requires more than just willpower. It requires preparation. The home environment plays a massive role in the “Care” aspect of our “Cure and Care” philosophy. When a home is adequately equipped, it reduces caregiver stress and increases patient safety.
However, walking into a medical supply store or browsing online can be overwhelming. There are thousands of gadgets, and it is hard to know what is a necessity and what is a luxury. Whether you are caring for an aging parent, managing diabetes, or recovering from a major surgery, having the right tools at your fingertips is crucial.
This guide provides a comprehensive, practical checklist of home health essentials. These are the items that bridge the gap between professional medical facilities and the comfort of your living room, ensuring safety, dignity, and effective management of chronic illness.
1. Monitoring Vital Signs
For many chronic illnesses—such as hypertension, heart disease, or respiratory issues—knowledge is power. You cannot manage what you do not measure. Having reliable home monitoring equipment lets you spot trends before they become emergencies.
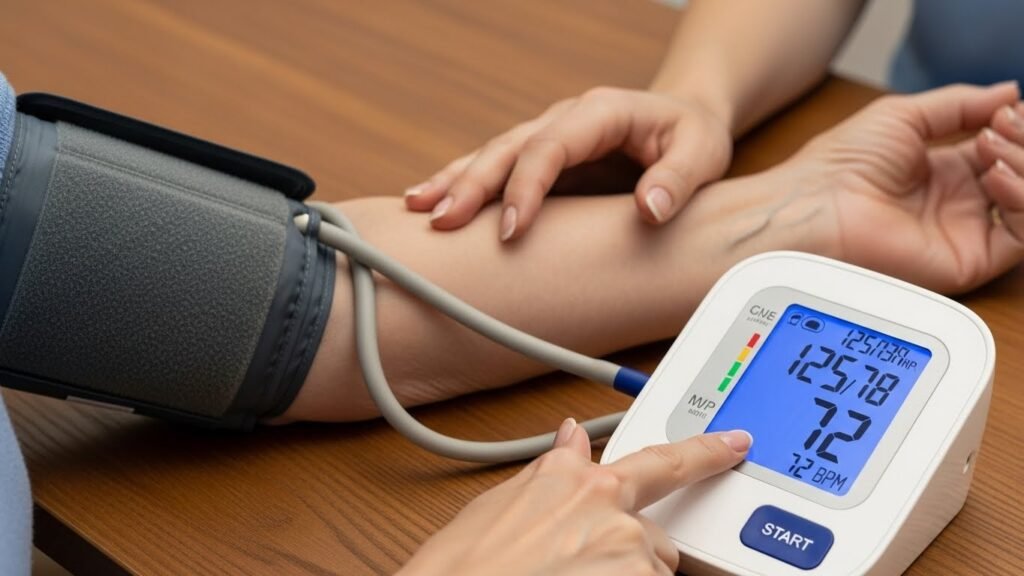
Digital Blood Pressure Monitor
High blood pressure is often called the “silent killer” because it has no apparent symptoms. A digital upper-arm monitor is generally more accurate than wrist models.
- Why you need it: To track daily fluctuations and provide your doctor with accurate data logs.
- Tip: Look for a model with a large display and a memory function that stores previous readings.
Pulse Oximeter
This small device clips onto a finger to measure oxygen saturation levels in the blood and pulse rate. Since the global pandemic, this has become a household staple.
- Why you need it: It helps monitor respiratory efficiency, especially for patients with COPD, asthma, or heart failure.
Non-Contact Thermometer
Fever is often the first sign of infection. Old-fashioned mercury thermometers are dangerous and slow.
- Why you need it: Infrared forehead thermometers allow you to check a sleeping patient’s temperature without waking them up.
2. Medication Management Systems
One of the most common causes of hospital readmission is “medication non-adherence”—simply put, missing doses or taking the wrong pills. When a patient is on five or six different medications, relying on memory is a recipe for disaster.
Weekly Pill Organizers
Simple plastic containers labeled with days of the week (and times of day: Morning, Noon, Night) are lifesavers.
- Why you need it: It provides a visual confirmation that medication has been taken. If the “Tuesday Morning” slot is empty, you know the dose was administered.
Medication Logbook or App
Technology is excellent, but a physical notebook is reliable and accessible to all family members and visiting nurses.
- What to record: Name of the drug, dosage, time taken, and any side effects noticed.
Pill Cutter and Crusher
Some pills are large and complex to swallow, especially for elderly patients.
- Safety Note: Always check with your pharmacist before crushing medication, as some time-release capsules must be swallowed whole.

3. Bathroom Safety and Hygiene
The bathroom is statistically the most dangerous room in the house for seniors and those with chronic illnesses. Wet surfaces and hard tiles make falls likely and devastating. Modifying this space is a top priority for home health safety.
Shower Chair or Bench
Fatigue is a significant issue for patients with chronic illness. Standing for a 10-minute shower can be exhausting and increase the risk of slipping.
- Why you need it: It allows the patient to bathe independently and safely while seated.
Raised Toilet Seat and Grab Bars
Standard toilets are often too low for people with knee or hip issues, making standing up difficult.
- Why you need it: A raised seat reduces the distance a patient needs to squat. Grab bars (screwed into studs, not suction cups) provide crucial leverage and support.
Non-Slip Mats
Place these inside the tub and on the floor outside the shower.
- Why you need it: To provide traction on slippery surfaces.

4. Mobility Aids
Maintaining mobility is key to preventing bedsores, muscle atrophy, and depression. However, moving must be done safely.
Walkers or Rollators
A rollator is a walker with wheels and a seat.
- Why you need it: It provides stability for walking and a built-in seat if the patient suddenly gets tired.
Transfer Belt (Gait Belt)
This is a wide belt worn around the patient’s waist.
- Why you need it: It gives the caregiver something firm to hold onto when helping a patient stand up or transfer from a bed to a chair. It prevents the caregiver from pulling on the patient’s arms, which can cause injury.
5. Comfort and Prevention Supplies
Managing chronic illness isn’t just about medical data; it is about daily comfort. If a patient is bedbound or spends a lot of time sitting, skin integrity becomes a significant concern.
Pressure Relief Cushions
Specialized foam or gel cushions for wheelchairs and armchairs.
- Why you need it: To distribute weight evenly and prevent painful pressure ulcers (bedsores).
Humidifier
Dry air can aggravate respiratory conditions and dry out skin.
- Why you need it: To maintain optimal humidity levels, making breathing easier and sleep more restful.
Adaptive Clothing
Clothing with Velcro closures or elastic waists instead of difficult buttons and zippers.
- Why you need it: It promotes independence, allowing patients to dress themselves, and makes it easier for caregivers to assist.

6. Emergency Preparedness Kit
When you are managing a chronic condition, emergencies are a “when,” not an “if.” You need to be ready to leave for the hospital at a moment’s notice.
The “Go-Bag”
Keep a bag packed near the door containing:
- Copies of insurance cards and IDs.
- A current list of all medications and allergies.
- A change of clothes and toiletries.
- Phone chargers.
- Advanced directives or Living Will documents.
Emergency Contact Sheet
Do not rely on your phone contacts. Post a physical list on the fridge.
- Includes: Doctor’s numbers, nearest neighbor, family members, and poison control.
7. Organization and Communication Tools
Finally, mental clutter can be just as damaging as physical clutter. Organizing the “business” side of healthcare is essential.
The Master Binder
Create a central binder that stays in the home.
- Sections: Medical history, appointment calendar, insurance statements, and doctor’s notes.
- Why you need it: When a new nurse or family member steps in to help, everything they need to know is in one place.

Conclusion
Creating a healing environment at home does not happen by accident. It takes planning and the right home health essentials. By equipping your home with these tools, you are doing more than just buying products; you are building a safety net.
These items empower patients to maintain their dignity and independence for as long as possible. They also provide caregivers with the peace of mind that comes from being prepared.
Remember, you do not need to buy everything on this list at once. Start with the safety essentials (bathroom and medication management) and build up your kit as needs arise. At Cure and Care, we believe that a well-prepared home is the foundation of a healthy life.




